I decided to follow up Brett by also ripping off a TV show for my final blog post title.
If I’m being honest, I signed up for this class only because it simultaneously fulfilled my capstone requirement along with my last chemistry elective for my major. And on top of that, it has no lab! Going in, I didn’t think my situation could get any better, but I found out some of my best friends were taking the class, so my excitement grew.

The way the class was set up was something I’ve never experienced before. The emphasis on reading and dissecting scientific papers helped me develop a skill that will help me in any future path I decide to take. Especially for the majority of students in our class going into a health vocation, it’s very important to not only be able to read and understand scientific literature, but to develop an interest and love for continuing their education so they can provide the best care for their patients as new research continues to develop.
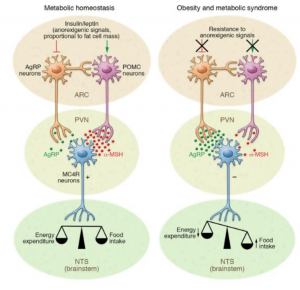
All of you know I became a little obsessed with the gut-brain connection during our time in this class. You’re probably wondering how I became interested, so I’ll give you a little background. Over the past couple of years, I got really into listening to lifestyle and health podcasts and reading books they recommend (Renegade Radio and The Cabral Concept are my two favorites). In almost every single podcast, they mention something about gut health and how it relates to the whole body.
I’m someone who’s had gut issues in the past, and it’s taken eliminating wheat and dairy as much as I can from my diet, along with other processed foods to eradicate the daily stomach pains. This, coupled with hearing so much in podcasts and books led me to dive deeper into the subject.
Neurochemistry allowed me to dive deep into the gut-brain connection, which instilled in me a love for learning about the topic. I would get excited every week to find out what the connection was between the topic we were researching and the gut, and to everyone’s surprise (not mine), there was always a connection. One of my favorite weeks was exploring the gut-brain connection in concussion, partly because at first nobody (but me) thought there could be any connection between the two whatsoever. The fact that traumatic brain injuries instantly disrupt the tight junctions of the intestinal epithelial layer is still baffling to me.
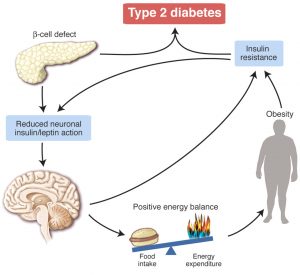
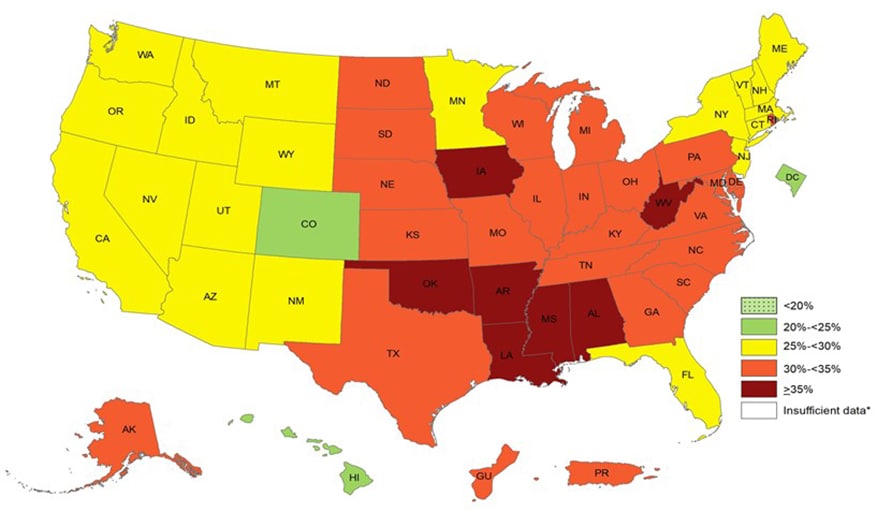
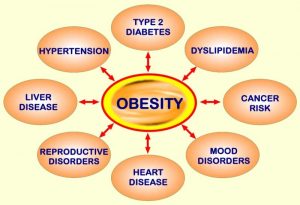
Another favorite week of mine was connecting diabetes to Alzheimer’s Disease. These are two diseases that are increasingly on the rise in the United States and will eventually become a crisis if trends continue the way they are. That particular week it struck me that most people aren’t educated on how these diseases come about or how to prevent them. If I ever end up becoming a health practitioner, I would educate all of my patients on these two diseases and teach them how preventable they are. Our class had some very good discussions about preventative medicine and what people can do to avoid all of the problems discussed in the papers we read. A large portion of our class is going into a health profession, and I think everyone learned something they can incorporate in their future career.
To speak more on the class itself, I was a big fan of how it wasn’t focused on constantly studying for a grade, but instead trying to break down a difficult topic to simpler terms and make connections to the real world and communicate that to others. I believe that is one of the most overlooked and valuable skills someone can have, not only simplifying a topic, but being able to communicate it to others. You always hear in every industry, the thing that separates someone from others and will get them promotions and more success is the ability to communicate effectively, along with just being a likable person. I think that skill is what Concordia really wants its students to come away with in their capstone experience, and Neurochemistry did exactly that. I was pushed to break down very difficult concepts and explain them a dozen times to my classmates every week, and then connect those concepts to other issues.
To conclude my commentary on Neurochemistry, I’d like to thank everyone in our class and Dr. Mach for a great class and some excellent conversations. I’ve come out of this class a better communicator, more knowledgeable, and more passionate about health and the gut-brain connection. I’d recommend this class to anyone at Concordia because I really believe everyone should know how to read scientific literature and develop their own opinions about it, rather than getting all of their information from biased sources, which is such commonplace today.


 College encourages liberal learning from the very first day you step foot on campus as a student. As freshmen are standing there wide-eyed in their bright yellow beanies, they are constantly reminded to “BREW.” If you are not from Concordia, I am assuming you are thinking of a different kind of brew. However, at Concordia, we understand BREW in a different context. To BREW means to become responsible engaged in the world. This concept is reinforced with Concordia’s five goals of liberal learning.
College encourages liberal learning from the very first day you step foot on campus as a student. As freshmen are standing there wide-eyed in their bright yellow beanies, they are constantly reminded to “BREW.” If you are not from Concordia, I am assuming you are thinking of a different kind of brew. However, at Concordia, we understand BREW in a different context. To BREW means to become responsible engaged in the world. This concept is reinforced with Concordia’s five goals of liberal learning.