The human brain is like a city under constant construction, with billions of cells building and connecting to form the networks that shape our thoughts, emotions, and perception of reality. This process depends on precise signals that tell cells where to go and what to do. Most of the time, everything comes together as it should, but when those signals are even slightly off, the brain can develop in ways that aren’t immediately visible yet have lasting effects on how the world is experienced. In conditions like schizophrenia, these early changes in brain development may play a key role in shaping how reality is perceived later in life.
The Science of Schizophrenia: Building (and Misbuilding) the Brain
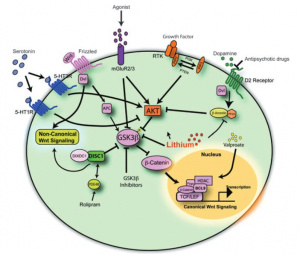
At the center of brain development are powerful signaling systems that guide how neurons grow, connect, and communicate. One of the most important of these is the Wnt signaling pathway, which helps control how brain cells develop and organize into functional networks. A key part of this pathway involves a protein called β-catenin. When Wnt signaling is active, β-catenin builds up and turns on genes that support healthy brain development. When the pathway is less active, another protein called glycogen synthase kinase-3β (GSK-3β) helps in the breakdown of β-catenin, preventing those genes from being expressed. This balance between activation and breakdown is critical, if it is disrupted, brain development can be altered.
This pathway is also closely connected to dopamine, a neurotransmitter often linked to schizophrenia. Dopamine plays a major role in motivation, reward, and perception, and imbalances in dopamine signaling are strongly associated with symptoms such as hallucinations and delusions. Emerging research suggests that dopamine and Wnt signaling may interact, meaning that disruptions in one system can influence the other. For example, changes in dopamine activity can affect GSK-3, which in turn impacts the Wnt pathway and brain development. Together, these overlapping systems highlight how schizophrenia may arise not from a single issue, but from interconnected changes in both brain signaling and structure [1].
What Brain Imaging Reveals
While molecular pathways like Wnt help explain what may be happening at a cellular level, brain imaging techniques like fMRI, DTI, and PET scans show how these changes appear in the brain itself. These tools reveal that schizophrenia is not limited to a single area, but instead involves multiple interconnected regions that support thought, emotion, and perception [1].
One of the most consistently affected areas is the prefrontal cortex, which is responsible for planning, attention, working memory, and decision making. In individuals with schizophrenia, this region often shows reduced activity, known as hypofrontality, along with decreased gray matter and weaker connectivity. These changes are strongly linked to cognitive and negative symptoms, such as concentrating and organizing thoughts.
The amygdala and hippocampus, which are involved in emotion and memory, are also significantly affected. Abnormal amygdala activity can contribute to heightened emotional responses, paranoia, and difficulty interpreting social cues. The hippocampus, often smaller and functionally altered, plays a role in memory and distinguishing internal thoughts from external reality, helping explain symptoms like hallucinations and delusions in schizophrenia [1].
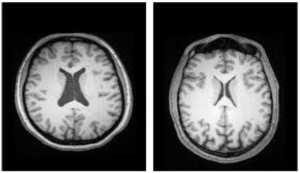
Disruptions are also seen in the thalamus, which normally acts as a relay center for sensory information. Reduced volume and impaired communication with cortical regions can lead to sensory misprocessing, hallucinations, and difficulty focusing attention. In addition, enlargement of the brain’s ventricles, one of the most consistent findings in schizophrenia, typically reflects a loss of surrounding brain tissue.
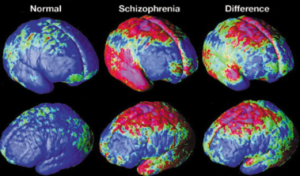
Beyond the regions discussed above, schizophrenia involves widespread changes throughout the brain. There is an overall decrease in both gray and white matter, leading to reduced connectivity between neurons. Decreased myelination slows communication between neurons, while increased brain inflammation may further disrupt signaling. Some research also suggests accelerated brain aging, with schizophrenic brains appearing 3.5 years older than neurotypical brains [3]. Together, these findings reflect that schizophrenia is a disorder of brain networks rather than a single isolated issue.
Why This Matters
Looking at schizophrenia through both a molecular and structural lens provides a more complete understanding of the disorder. The Wnt signaling pathway helps guide brain development and connectivity, and when this pathway is disrupted, it may contribute to the structural and functional brain differences observed in schizophrenia. In other words, if the signals that guide how the brain is built are altered, the result may be a brain that is wired differently from the start. Understanding schizophrenia in this way shifts the focus from simply treating symptoms to understanding the underlying biology. By studying pathways like Wnt, researchers may be able to develop more targeted treatments that address the root causes of the disorder rather than just its outward symptoms. As research continues, this approach may lead to earlier detection, better treatment options, and improved outcomes for individuals living with schizophrenia.
References
[1] K. Singh, “An emerging role for Wnt and GSK3 signaling pathways in schizophrenia,” Clinical Genetics, vol. 83, no. 6, pp. 511–517, Apr. 2013, doi: https://doi.org/10.1111/cge.12111.
[2] R. E. Team, “The Neurobiology of Schizophrenia: Brain Regions Explained,” ReachLink, Jul. 25, 2025. https://reachlink.com/advice/schizophrenia/neurobiology-of-schizophrenia-brain-regions-explained/
[3] A. Kandola, “How does schizophrenia affect the brain?,” Medicalnewstoday.com, Jan. 30, 2023. https://www.medicalnewstoday.com/articles/what-part-of-the-brain-is-affected-by-schizophrenia#affected-regions
[4] A. Saha, S. Park, Zong Woo Geem, and P. K. Singh, “Schizophrenia Detection and Classification: A Systematic Review of the Last Decade,” Diagnostics, vol. 14, no. 23, pp. 2698–2698, Nov. 2024, doi: https://doi.org/10.3390/diagnostics14232698.
[5] “Nature Reviews Neuroscience – Highlights,” Ucla.edu, 2025. http://users.loni.ucla.edu/~thompson/MEDIA/PNAS/NRN.html
Featured image created by Julia Wolf and ChatGPT
