The Silent Risks of Schizophrenia
Schizophrenia is a mental health condition that is thought to be a disorder of brain development and neural connectivity [2]. Symptoms of Schizophrenia typically show up in one’s early twenties however, the origins of Schizophrenia can begin during brain formation as a fetus [1][2].
Maternal Immune Activation
One of the lesser-known risk factors of schizophrenia is Maternal Immune Activation (MIA). This occurs when a pregnant person experiences an infection and their immune system responds by releasing cytokines. Cytokines are protective signaling molecules that help with regulating immunity. However, these cytokines can cross through the placenta and affect brain development [3]. One cytokine in particular, interleukin-8, is linked to schizophrenia [4]. This exposure to cytokines can alter how neural circuits form, specifically the Wnt pathway, during critical periods of development [2].
It is commonly known that sickness causes immune response, but did you know that environmental factors such as pollution from highways and microplastics can also trigger an immune response? [5] This Immune activation occurs without noticeable illness which can pose a risk to the developing brain of the fetus.
Timing also matters. Immune activation poses more of a significant risk during the first and second trimester of pregnancy [8]. This is when foundational neural circuits and brain structures being formed. Even subtle disruptions during this time can have long-term effects.
Maternal immune response is also associated with other neurodevelopmental and neuropsychiatric conditions including ADHD and Autism spectrum disorder [6]. This suggests that there is a shared neurodevelopment pathway where similar disruptions can result in different outcomes depending on genetics and life experiences.
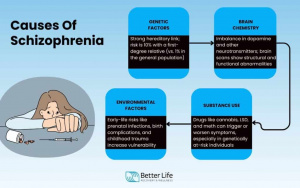
Image sourced from BetterLife
Genetic Vulnerability
Environmental factors do not act alone. Instead, they interact with one’s genetics to influence the risk of schizophrenia. Genetic variations involved in immune function, brain development and systems like Wnt/GSK3 signaling. While certain genetics can increase vulnerability, an environmental trigger would have to play a role for there to be alterations in brain development [7].
Genetics make up 80% of schizophrenia risk. A child with two affected parents has a 40% prevalence while a child with one affected parent has a 12% prevalence [9]. Changes in brain chemicals like glutamate and dopamine may also play a part in schizophrenia prevalence [10].
Image sourced from PatientsEngage

Changing How We Think About Schizophrenia
Schizophrenia is not a sudden or random condition. It occurs because of brain development and genetics before symptoms appear.
Many of these risk factors are out of one’s control since processes like immune activation are normal and necessary to protect the body. This shows that schizophrenia is not a result of personal failures. It’s important that as a society, we create more understanding to help reduce the stigma.
What appears later in life reflects subtle changes that had occurred in brain development [2]. By understanding these hidden risks, we can move closer to understanding how the brain develops to develop prevention measures and treatments.
Sources:
- Schizophrenia: Symptoms, causes & treatment options | nami. (n.d.). Retrieved March 25, 2026, from https://www.nami.org/types-of-conditions/schizophrenia/#:~:text=Although%20schizophrenia%20can%20occur%20at%20any%20age%2C,is%20possible%20to%20live%20well%20with%20schizophrenia
- Singh, K. K. (2013). An emerging role for Wnt and GSK3 signaling pathways in schizophrenia.Clinical Genetics, 83(6), 511–517. https://doi.org/10.1111/cge.12111
- Ayoub, G. (2025). Neurodevelopmental impact of maternal immune activation and autoimmune disorders, environmental toxicants and folate metabolism on autism spectrum disorder.Current Issues in Molecular Biology, 47(9), 721. https://doi.org/10.3390/cimb47090721
- Ellman, L. M., Deicken, R. F., Vinogradov, S., Kremen, W. S., Poole, J. H., Kern, D. M., Tsai, W. Y., Schaefer, C. A., & Brown, A. S. (2010). Structural brain alterations in schizophrenia following fetal exposure to the inflammatory cytokine interleukin-8.Schizophrenia Research, 121(1–3), 46–54. https://doi.org/10.1016/j.schres.2010.05.014
- Yang, W., Jannatun, N., Zeng, Y., Liu, T., Zhang, G., Chen, C., & Li, Y. (2022). Impacts of microplastics on immunity.Frontiers in Toxicology, 4, 956885. https://doi.org/10.3389/ftox.2022.956885
- Cattane, N., Richetto, J., & Cattaneo, A. (2020). Prenatal exposure to environmental insults and enhanced risk of developing Schizophrenia and Autism Spectrum Disorder: Focus on biological pathways and epigenetic mechanisms.Neuroscience & Biobehavioral Reviews, Prenatal Stress and Brain Disorders in Later Life, 117, 253–278. https://doi.org/10.1016/j.neubiorev.2018.07.001
- Wahbeh, M. H., & Avramopoulos, D. (2021). Gene-environment interactions in schizophrenia: A literature review.Genes, 12(12), 1850. https://doi.org/10.3390/genes12121850
- Mor, G., Cardenas, I., Abrahams, V., & Guller, S. (2011). Inflammation and pregnancy: The role of the immune system at the implantation site.Annals of the New York Academy of Sciences, 1221(1), 80–87. https://doi.org/10.1111/j.1749-6632.2010.05938.x
- Causes and risk factors of schizophrenia. (n.d.). Clínic Barcelona. Retrieved March 25, 2026, from https://www.clinicbarcelona.org/en/assistance/diseases/schizophrenia/causes-and-risk-factors
- Mayo Clinic. (n.d.). Schizophrenia: Symptoms and causes. Retrieved March 25, 2026, from https://www.mayoclinic.org/diseases-conditions/schizophrenia/symptoms-causes/syc-20354443
Cover image sourced from ChatGPT
