Obviously, cannabis, weed, marijuana, etc. and its legalization have been a controversial, polemic, political hot button for the past 40+ years. However, this stigma and demonization of the cannabis plant, and its psychoactive product: marijuana, has resulted in many misconceptions and confusion about how they actually work. Misunderstanding and fear have caused claims like, “weed melts your brain cells” which can be a dangerous misconception. Why would it be dangerous? Because a brain melting drug is terrifying and the psychoactive ingredient in marijuana, THC, does not melt brain cells, at all.
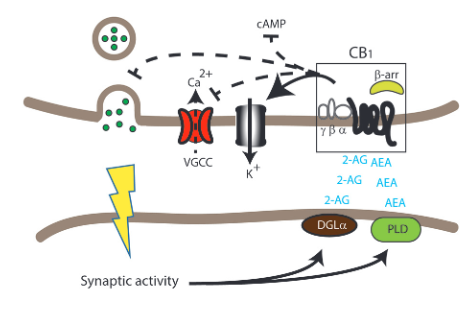
So how does marijuana actually work in the brain? Let’s focus on THC, the most active part of marijuana. THC is the drug that is active in the brain which can be said to be psychoactive. THC works by binding to proteins in the endocannabinoid system. Endocannabinoids? We have marijuana products in our brains?!? No, not quite. The endocannabinoid system was coined that because scientists discovered it by seeing which proteins cannabis binds to. The endo- part is in reference to the small endogenous (naturally occuring in the body) molecules that bind to these receptors.
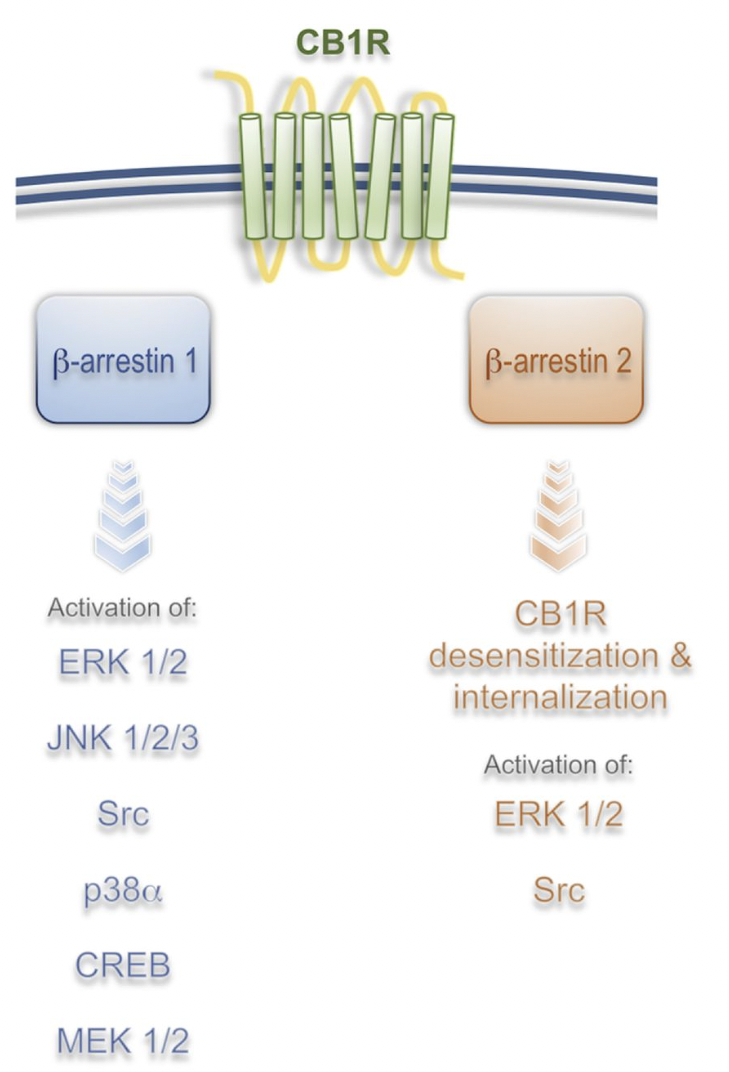
What are these mysterious receptors? There are two receptors and they are known as CB1 and CB2. CB = Cannabinoid. The figure below from this pharmacy explains quite well the differences in the two receptor types, their function, and their locations in the body.
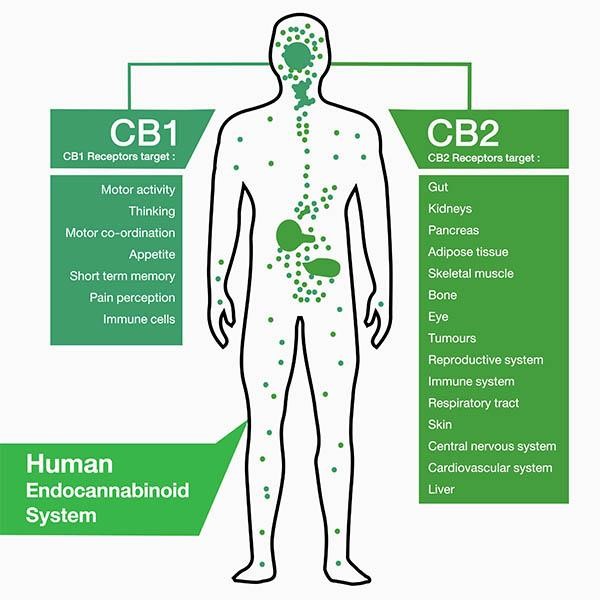
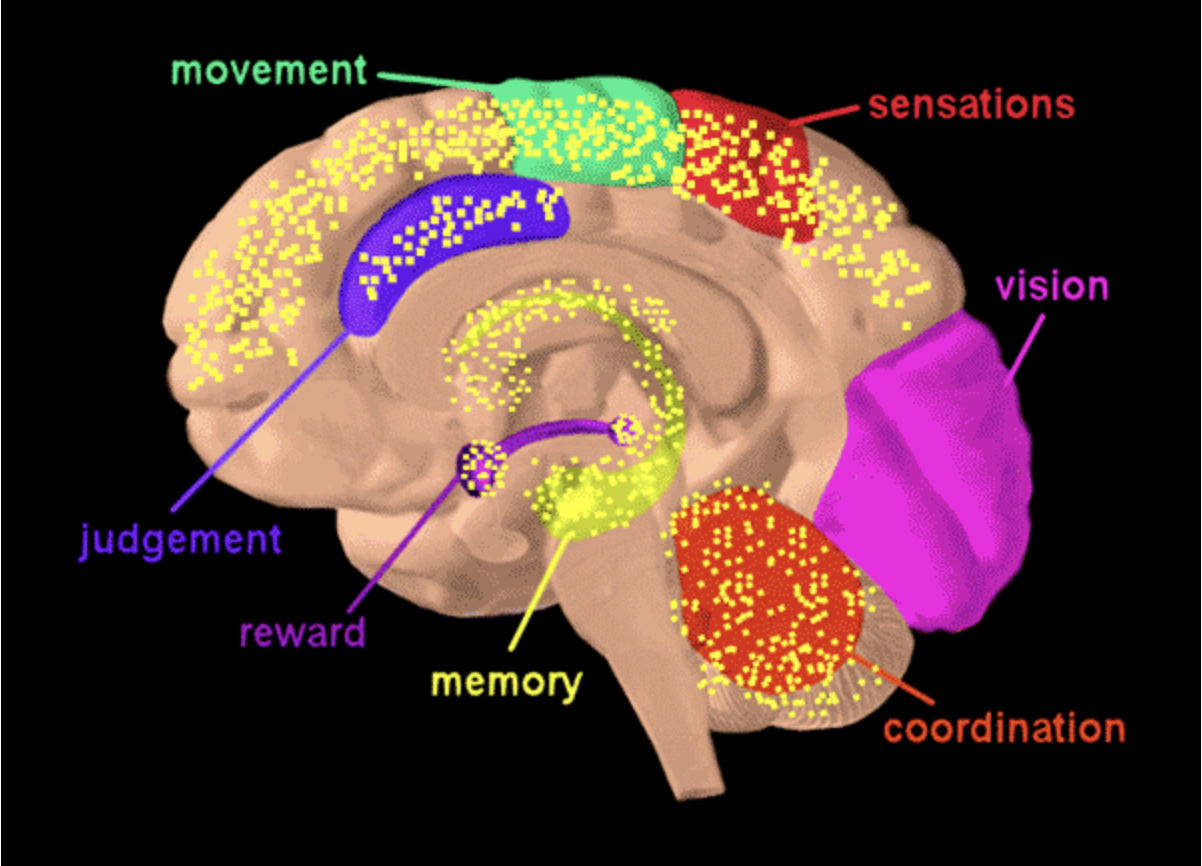
THC or Tetrahydrocannabinol, like was mentioned before, is the most potent psychoactive ingredient in weed/cannabis. THC binds mostly to the CB1 receptors. Knowing this, we can start to see how some of the common symptoms of smoking weed or ingesting THC could arise. Looking at the figure above, we can see CB1 targets pain perception which we can connect to how some people use cannabis for pain. Additionally, CB1 impacts appetite, if we think about how people commonly get the “munchies” or temporarily increased appetite while using cannabis, now we can see how to connect THC to the CB1 receptor to then appetite.
Tetrahydrocannabinol (THC)
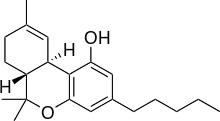
Next let us learn about what are these endogenous molecules, or ligands, that would bind to these receptors in a normally functioning brain.
Anandamide (AEA)

2-Arachidonoylglycerol (2 – AG)

Above the paragraph, these two molecules are the main ligands, AEA and 2-AG. Now a chemical structure can be intimidating, but the function of these molecules is relatively simple. They are messengers that will attach to the CB receptors that result in signals sent in the brain. When these endogenous ligands are used instead of THC or CBD, the endocannabinoid system works on regulating the body, whether that be hunger, temperature, energy, and so many more.
Nevertheless, the key to how THC and CBD are active in the brain and body is the endocannabinoid system. However, the endocannabinoid system is no boogeyman that should be demonized and feared like cannabis has in the past; it is a natural part of the body’s functions in and outside of the brain.
References:
Artstract made in Canva
Kendall, D. A., & Yudowski, G. A. (2017). Cannabinoid Receptors in the Central Nervous System: Their Signaling and Roles in Disease. Frontiers in Cellular Neuroscience, 10. https://doi.org/10.3389/fncel.2016.00294
Endocannabinoid System: A Simple Guide to How It Works. (2019, May 17). Healthline. https://www.healthline.com/health/endocannabinoid-system
Mosher, C. J., & Atkins, S. (2020). In the Weeds: Demonization, Legalization, and the Evolution of US Marijuana Policy. Social Forces, 98(4), 1–3. https://doi.org/10.1093/sf/soaa003
MD, P. G. (2021, August 11). The endocannabinoid system: Essential and mysterious. Harvard Health. https://www.health.harvard.edu/blog/the-endocannabinoid-system-essential-and-mysterious-202108112569
What is the Endocannabinoid System? | Sona Pharmacy + Clinic. (2020, April 1). https://sonapharmacy.com/what-is-the-endocannabinoid-system/
2-Arachidonoylglycerol. (2023). In Wikipedia. https://en.wikipedia.org/w/index.php?title=2-Arachidonoylglycerol&oldid=1165555760
Anandamide. (2024). In Wikipedia. https://en.wikipedia.org/w/index.php?title=Anandamide&oldid=1211788315


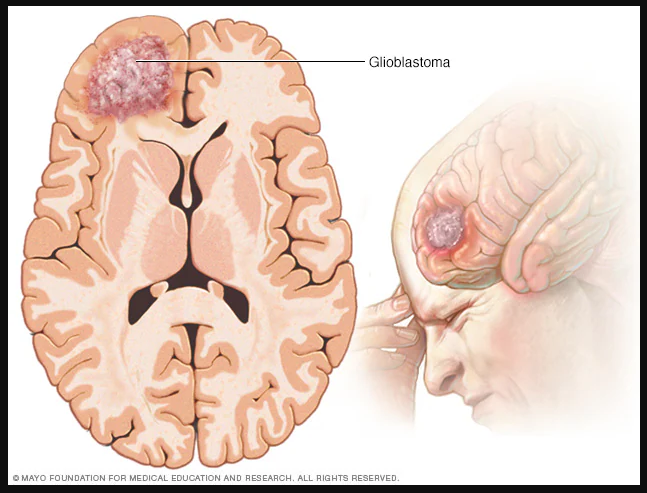

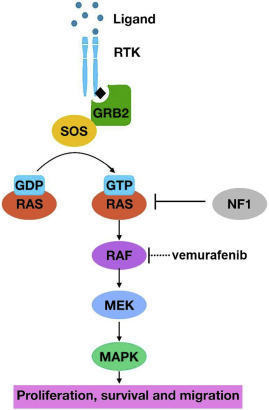

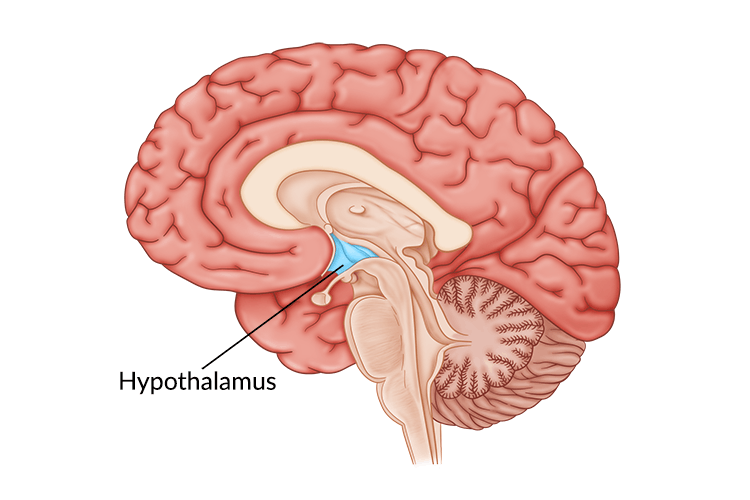
 Figure 1: Diagram of the brain with the hypothalamus highlighted in blue. The hypothalamus is deep in the central part of the brain.
Figure 1: Diagram of the brain with the hypothalamus highlighted in blue. The hypothalamus is deep in the central part of the brain.