WHAAAM!!!!
Congratulations. Whether from a head-to-head athletic collision, tripping backward on slippery ice, or the result of an unfortunate car accident, you have just joined the millions of Americans who will experience a concussion in a typical year.
I understand you might have questions, and they’re good ones (what was I doing running on ice, why am I in this ridiculous thought experiment, can’t you think of a better attention-grabber) but the important thing right now is to rest and recover. In fact, you probably shouldn’t be reading this short article, in fact, you probably shouldn’t be doing anything at all…you see, our treatment options for concussion are limited to rest…and Tylenol for headaches. Yes, you heard me right, one of the most common neurological injuries has the same treatment options as a twisted ankle—minus the ice. Put another way, there are no current drugs available to help treat concussion.

I know this may sound shocking and/or disheartening, but, before you go, I’d like to share one glimmer of hope, because there’s some promising new research for treating concussion. To understand how this drug, called ILB, works we’ll need a super short primer on the neuroscience of concussion.
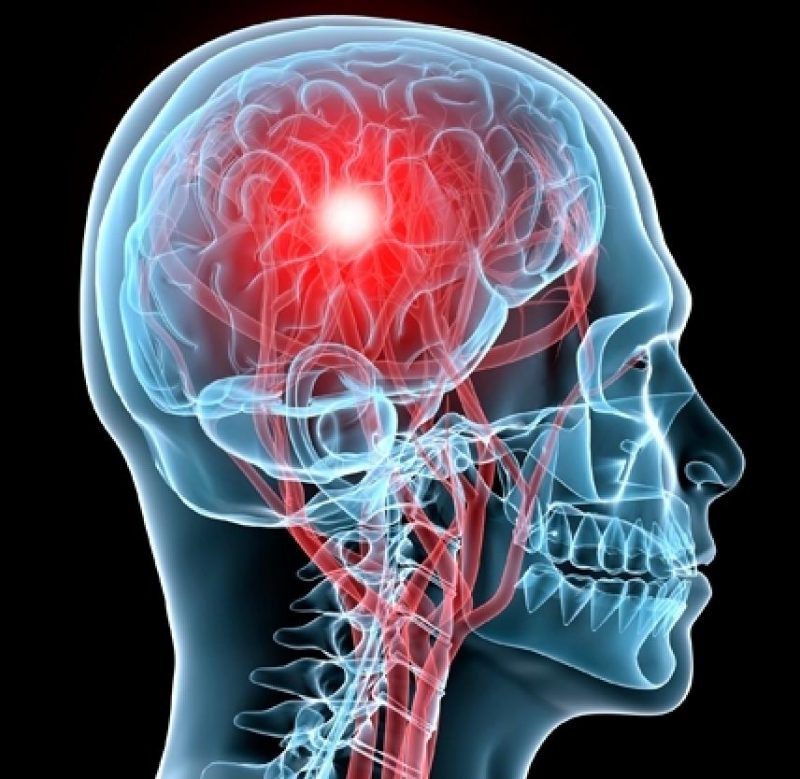
Your Brain on Concussion

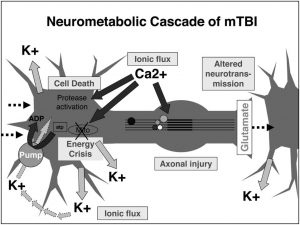
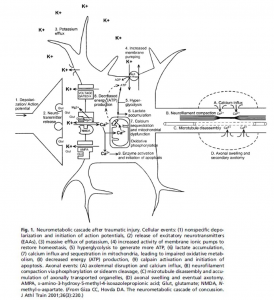
As your skull impacted the hard surface of another person, the ground, or your car window, a couple things happened in a very short amount of time. First, your body went from accelerating to immobile very quickly, causing your brain to slam into your skull and slosh around a bit inside. Zooming in, this force causes trauma to the membranes of your axons (the long, message sending bits of neurons). This in turn causes an imbalance in ion levels in and around the affected neurons, as the microscopic tears in axon membranes allow potassium ions to leave and calcium ions to enter with no regard for typical entrance/exit policies. Calcium, being the potent messenger that it is, goes around turning all sorts of things on and off that it shouldn’t, a bull let into a china shop by an earthquake. This disrupts the delicate neuronal balance even further, forcing membrane pumps to go into overtime trying to reestablish normal ion levels. As you might imagine, pumping a whole bunch of ions against their concentration gradient is tough work (think bailing out a canoe that’s taking on water), so naturally, this process uses up a ton of cellular energy (ATP). Normally, the neuron’s ATP-generating mitochondria (the famous powerhouses of the cell) can handle surges in energy demand, but our dear friend calcium has been sequestered in the mitochondria to prevent it from doing more cellular damage. While temporarily locking calcium in the mitochondria is an effective stop-gap measure, the downside is it hampers energy production. These dysfunctional mitochondria, coupled with increased neuroinflammation and reactive oxygen species (ROS) generation further exacerbate the low-energy crisis in traumatized neurons, culminating in neuron death.

The take-home message from diving into the concussed brain is that physical head trauma leads to a neuronal energy crisis, and prolonged low-energy states increase the amount of cell death and subsequent recovery time.
The trauma-induced energy crisis presents a critical unmet need to produce treatments that help to restore the neuronal energy balance so neurons affected by concussion can heal and repair.
This is where the good news comes in. Hot off the press is a 2020 article demonstrating that dextran sulfate (ILB: a low-weight carbohydrate) restores brain energy after traumatic brain injury (TBI) in rats. Johansson et. al (2020)., use N-acetyl aspartate (NAA) as a proxy energy metabolite (If NAA goes up, then brain metabolism must be up) to measure the effectiveness of the ILB treatment.

This data shows that ILB increases NAA levels (orange and red graphs) in rats following TBI! Yay!
Now, before you rush off and call your doctor for some ILB, a few caveats:
- This data is in rats, not humans, rigorous clinical trials are required to ensure the drug’s efficacy and safety in humans
- The model was of severe TBI, concussion is categorized as mild TBI so the effect seen may or may not translate—more research needed!
- It’s still unclear exactly how ILB causes increased NAA, it could be by directly improving mitochondrial function, lowering neuroinflammation and/or ROS generation, or some combination of the three. In any case, the mechanism of action should be better explained before we go popping ILB pills in humans.
All said, while rest is still the gold standard “treatment” for concussion (because resting your brain prioritizes neuronal healing instead of other physical/mental tasks), ILB represents an exciting new development for concussion treatment! Now turn off your phone and rest your brain!




 effects of rapamycin that was found was that, when intermittently administered, rapamycin led to stem cell regeneration. Considering some of the applications for stem cells, this is an amazing discovery that could have far reaching implications on the future of medicine. And that’s potentially just the tip of the iceberg. Because of the mTOR1 inhibition through rapamycin, it has been found that there is a decreased risk of cancer, since mTOR1 signaling can lead to cell proliferation. Tumor regression has also been observed to occur. It’s also been found that mTOR1 signalling sometimes leads to misfolded proteins. Using rapamycin, inhibiting mTOR1 led to greater autophagy and suppression of protein synthesis, which is important because this means that rapamycin can have neuroprotective effects in not just Alzheimers, but also Parkinson’s Disease and Huntington’s Disease.
effects of rapamycin that was found was that, when intermittently administered, rapamycin led to stem cell regeneration. Considering some of the applications for stem cells, this is an amazing discovery that could have far reaching implications on the future of medicine. And that’s potentially just the tip of the iceberg. Because of the mTOR1 inhibition through rapamycin, it has been found that there is a decreased risk of cancer, since mTOR1 signaling can lead to cell proliferation. Tumor regression has also been observed to occur. It’s also been found that mTOR1 signalling sometimes leads to misfolded proteins. Using rapamycin, inhibiting mTOR1 led to greater autophagy and suppression of protein synthesis, which is important because this means that rapamycin can have neuroprotective effects in not just Alzheimers, but also Parkinson’s Disease and Huntington’s Disease.  Before we all start taking insulin, it’s important to remember however that one of the most consequential aspects of a drug’s effects and effectiveness is the dosage and how often its administration. With rapamycin, the appropriate ratios of both of these factors are still unknown as of yet, but research is being done to try decipher further how to access the perceived positive effects of the drug. It has been seen though that rapamycin doesn’t fully inhibit mTORC1 processes, and so a combination with another treatment would more effectively implement the positive effects of Rapamycin.
Before we all start taking insulin, it’s important to remember however that one of the most consequential aspects of a drug’s effects and effectiveness is the dosage and how often its administration. With rapamycin, the appropriate ratios of both of these factors are still unknown as of yet, but research is being done to try decipher further how to access the perceived positive effects of the drug. It has been seen though that rapamycin doesn’t fully inhibit mTORC1 processes, and so a combination with another treatment would more effectively implement the positive effects of Rapamycin. increase insulin resistance, but the mechanism for why this occurs is speculated to be known (inhibition of mTOR2). Other negative effects included increased hyperglycemia within type 2 diabetes mouse models, and the ability for tumors to start regrowing after treatment with rapamycin stopped.
increase insulin resistance, but the mechanism for why this occurs is speculated to be known (inhibition of mTOR2). Other negative effects included increased hyperglycemia within type 2 diabetes mouse models, and the ability for tumors to start regrowing after treatment with rapamycin stopped.


 In The Brain
In The Brain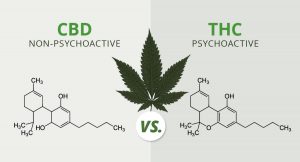 CBD Vs. THC?
CBD Vs. THC?
 develop depressive symptoms afterward, which is quite a dramatic number. Another fact that was found is equally concerning: one study found that after only a mild traumatic brain injury, there was a 15% chance that the person developed major depression. This is the lightest and least serious type of brain injury (which you can get simply by hitting your head slightly too hard) and the worst, most serious type of depression, occurring in more than 1 in 7 people who experience a concussion. This is significant not only because of the depression part, but because this points to concussion as being more than purely “an annoyance”. In fact, the total prevalence across all severities of TBIs for major depression is 14-29%. In other words, up to a third of people who experience a concussion develop the clinically-worst type of depression.
develop depressive symptoms afterward, which is quite a dramatic number. Another fact that was found is equally concerning: one study found that after only a mild traumatic brain injury, there was a 15% chance that the person developed major depression. This is the lightest and least serious type of brain injury (which you can get simply by hitting your head slightly too hard) and the worst, most serious type of depression, occurring in more than 1 in 7 people who experience a concussion. This is significant not only because of the depression part, but because this points to concussion as being more than purely “an annoyance”. In fact, the total prevalence across all severities of TBIs for major depression is 14-29%. In other words, up to a third of people who experience a concussion develop the clinically-worst type of depression. 

 The app essentially functions as a gamified symptoms journal, where concussed individual reports symptoms and feelings, then the app turns those inputs into a game-like version of their feelings. This can help avoid social isolation associated with concussion recovery, especially since concussion patients are urged not to do anything that may be detrimental to their recovery. Within the app, users could form a network around their symptom log and comment and interact with other users’ posts, generating a cohesiveness between patients that may be looking for some more interaction when able. The main takeaway here is that, while you shouldn’t be overstimulating your brain and harming recovery, you can use what little screen time you have in a positive manner, leading to a more efficient recovery.
The app essentially functions as a gamified symptoms journal, where concussed individual reports symptoms and feelings, then the app turns those inputs into a game-like version of their feelings. This can help avoid social isolation associated with concussion recovery, especially since concussion patients are urged not to do anything that may be detrimental to their recovery. Within the app, users could form a network around their symptom log and comment and interact with other users’ posts, generating a cohesiveness between patients that may be looking for some more interaction when able. The main takeaway here is that, while you shouldn’t be overstimulating your brain and harming recovery, you can use what little screen time you have in a positive manner, leading to a more efficient recovery.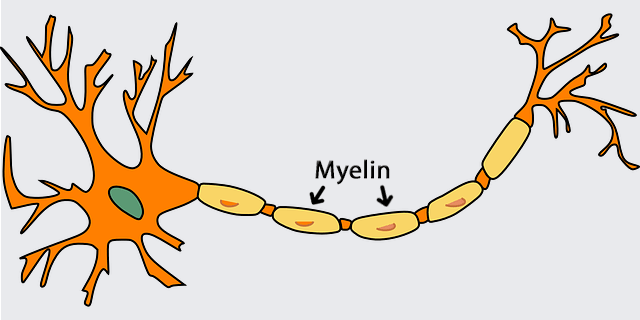
 from behind, let’s examine what occurred microscopically inside of his brain as a result. The sudden movement inside his skull most likely started out with neurons becoming “leaky”, or more permeable for ions to flow in/out of the cell. For TBIs, there is an extreme influx of calcium and sodium ions with an efflux of potassium ions.
from behind, let’s examine what occurred microscopically inside of his brain as a result. The sudden movement inside his skull most likely started out with neurons becoming “leaky”, or more permeable for ions to flow in/out of the cell. For TBIs, there is an extreme influx of calcium and sodium ions with an efflux of potassium ions.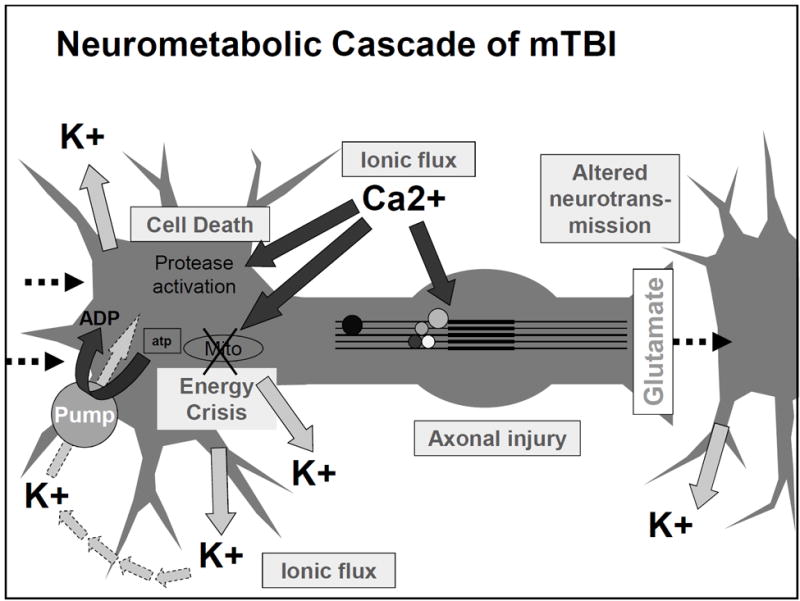 body compared to the amounts being consumed intracellularly results in an unfavorable side product being formed with ATP (lactate) and extra calcium getting stored in the mitochondria. Shrinking and running out of options, these cells quickly realize that they are now only doing more harm than benefit and decide to turn to apoptosis: programmed cell death.
body compared to the amounts being consumed intracellularly results in an unfavorable side product being formed with ATP (lactate) and extra calcium getting stored in the mitochondria. Shrinking and running out of options, these cells quickly realize that they are now only doing more harm than benefit and decide to turn to apoptosis: programmed cell death.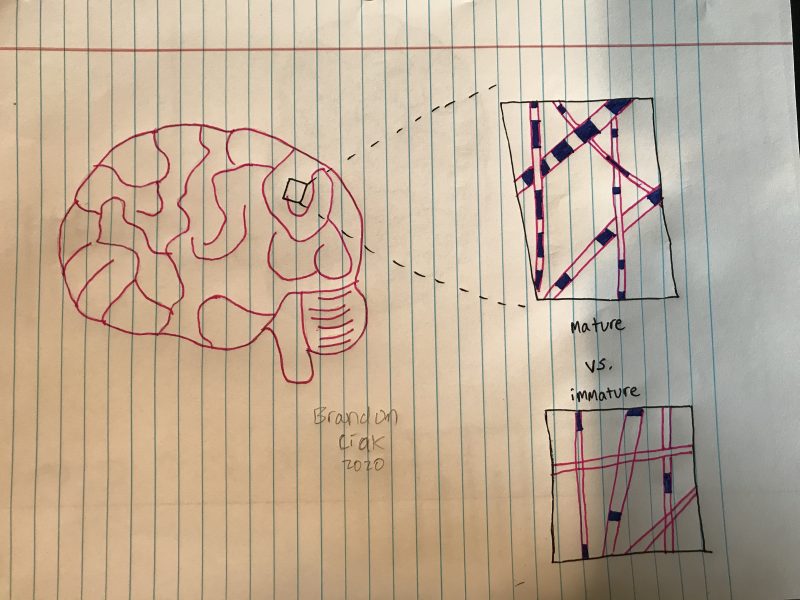 disruptions.
disruptions.