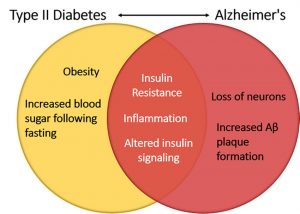
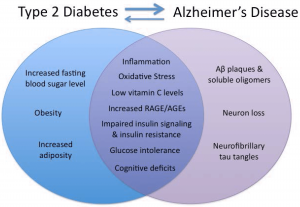
Alzheimer‘s disease or AD is a degenerative disease that leads to memory loss, and decline of cognitive functions. Type 2 diabetes (T2D) is caused by problems due to insulin resistance. How are these two different diseases related? Is glucose regulation related to neurons dying? Research has shown that having type 2 diabetes is a major risk factor for AD, and vice verses. These two diseases are more alike than they appear. The inflammation and insulin pathway are two molecular mechanisms that explain the correlation between the two diseases.
The Insulin Pathway
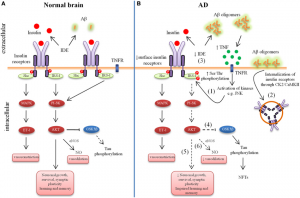
In order to understand the insulin pathway w e must first talk about insulin resistance. This resistance takes place in both AD and type two diabetes.
e must first talk about insulin resistance. This resistance takes place in both AD and type two diabetes.
Type 2 Diabetes: In order to breakdown glucose the body needs insulin. In T2D insulin does not work properly. This leads to high levels of glucose in the body, which causes high blood sugar. Having problems with insulin production can lead to other problems in the body, like in the brain for example.
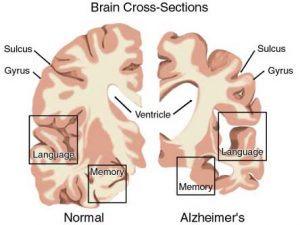
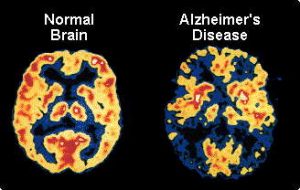
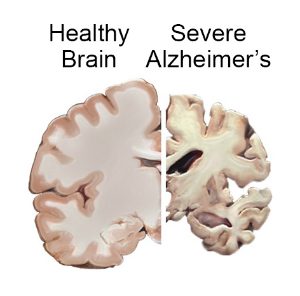
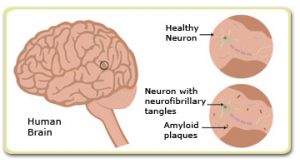
Alzheimer’s: Insulin resistance can be shown in postmortem brains of people who suffered from AD. This impaired insulin signaling can be seen clearly in the hippocampus region of the brain. It is thought that insulin resistance in an AD brain may be caused by the build up of amyloid beta plaques. However, this is one hypothesis. There are many more hypotheses being developed surrounding the topic of insulin resistance in the brain.
Inflammation
Insulin resistance plays a large role in the inflammation found in type 2 diabetes, and AD.
Type 2 Diabetes: Obesity, due to poor diet is often linked to the development of insulin resistance, and ultimately T2D. When fat cells accumulate, inflammatory cells follow. One of the main inflammatory cells involved in T2D is the cytokine TNF-α.
Alzheimer’s: Chronic inflammation is one of the characteristics of AD. The inflammation seen in AD is caused by the immune cell called microglia. The microglia are responsible for the protection and remodeling of synapses in the brain, and help contribute to neuroplasticity. Microglia often produce inflammatory cells in response to increased accumulation of amyloid beta plaques. Research has shown that in order for amyloid beta to cause insulin resistance, and therefore inflammation the cytokine TNF-α must be present.
What does this have to do with my diet?
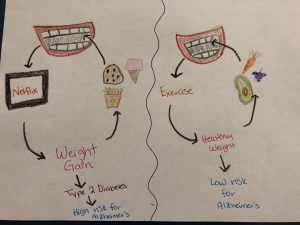
Our society values convenience, so when given the choice between fast food and taking the extra time to pack food it is not surprising that many of us would choose the fast food option. These poor dietary choices combined with spending your free time watching Netflix can lead to serious problems. Nearly 40% of Americans are obese, and 30% of those who are overweight or obese have type 2 diabetes. While maybe these statistics alone aren’t enough to change your mind maybe this next statistic will make you question whether that extra piece of cake is truly worth it. Having T2D doubles your chances of developing Alzheimer’s Disease. Now I am not saying to ditch fast food entirely, I enjoy treating myself too, but the next time I am given the option of packing my lunch or get fast food, I’ll be packing my own.
Why should you care?
There is no cure for Alzheimer’s Disease, so it is important to take preventative steps now. Remember, little changes can make all the difference.
- Pack a meal for on the go instead of getting fast food
- Watch TV or Netflix while you work out
- Find health snacks that you enjoy
- Take time for yourself!! Whether it by cooking dinner, or working out try to find healthy practices to implement now. Trust me, your future self will thank you.
Image 1 https://www.psychologytoday.com/us/blog/diagnosis-diet/201609/avoiding-alzheimer-s-disease-could-be-easier-you-think










 dementia cases, according to the Alzheimer’s Association. Unfortunately, the cause of AD is still not greatly understood despite years of research. This is mainly because of the multiple factors that contribute to AD. With other diseases, researchers have found one to two causations for that disease. But AD has so many possible causations that there is no set cure. Symptoms for AD include difficulty in remembering events, in finding commonly used words, in multiple-step tasks as well as signs of depression, agitation, and apathy.
dementia cases, according to the Alzheimer’s Association. Unfortunately, the cause of AD is still not greatly understood despite years of research. This is mainly because of the multiple factors that contribute to AD. With other diseases, researchers have found one to two causations for that disease. But AD has so many possible causations that there is no set cure. Symptoms for AD include difficulty in remembering events, in finding commonly used words, in multiple-step tasks as well as signs of depression, agitation, and apathy.  Diabetes. However, in contrast to Alzheimer’s Disease, people with Type 2 Diabetes can manage their disease well by exercise, a healthy diet, and insulin therapy and medication.
Diabetes. However, in contrast to Alzheimer’s Disease, people with Type 2 Diabetes can manage their disease well by exercise, a healthy diet, and insulin therapy and medication.