Just three weeks ago, I purchased A Brief History of Time, by Stephen Hawking, and less than two weeks ago, I finished the book. From what I hear, Stephen Hawking’s persona is equally linked to ALS (amyotrophic lateral sclerosis) as it is to black holes, quantum mechanics, and general relativity. The “pop culture” idea of the man is as the wheelchair-bound genius. Thus, I found it remarkably coincidental that the following Monday I was required to read a recent journal review of ALS for my neurochemistry course.

The review highlighted recent research regarding RNA dysregulation and oxidative stress as main culprits for the debilitating disease. It insisted that the two were inexplicably linked through the processes of two nuclear (i.e. pertaining to the nucleus of the cell) proteins, FUS and TDP43. The overarching theory was that oxidative stress would cause these proteins to leave the nucleus, and find their way to other parts of the cell where they would cause problems with RNA (think of it as the link between DNA and proteins). Basically, oxidative stress was destroying the cell’s ability to properly make proteins. This would in turn lead to more oxidative stress which would just start the cycle over again, eventually the cell (a motor neuron, the body’s way of telling muscles to move) would die, and thus we have ALS.
This is truly a remarkable theory, and certainly there is evidence to support it, but there is a competing theory: excitotoxicity of motor neurons. Excitotoxicity is a big word. It means that the cell is getting too much stimulation, and thus eventually dies. (Too much of anything is bad it may seem.) Indeed, the best pharmaceutical drug prescribed to ALS, riluzole, is a glutamatergic inhibitor (prevents excitotoxicity). However, even this drug is thought to extend the average life expectancy of a patient, which is only 2-3 years usually, by only a few extra months.

If the drug works at all, it must be targeting something that is causing the disease, so we can readily assume that excitotoxicity is a culprit. But the drug certainly does not cure ALS, so it cannot be giving us the full story. Perhaps the review I mentioned gives the other half of the story, though that is highly doubtful. In the end, we must agree that there is no single answer to solving this problem.
I then look back at Hawking, and his book, A Brief History of Time, and again notice a coincidence. Hawking argues that our knowledge of the universe is likewise incomplete, as there may indeed be no singular answer to the problem. He argues for more collaboration, and ultimately more research. If this is to be the case, however, I wonder if perhaps our research into the workings of the universe would be misplaced.

Let us imagine, for a second, what kind of world we would live in if instead of wasting hours on end mathematically modeling the trajectories of black holes spiraling into one another, we put our efforts into saving lives medically. We spend enormous amounts of time on understanding the maddeningly large, and the unthinkably small, that we forget about the in-between where lives may be saved. How is it that we can say how much slower time may progress for a relativistic traveler, but we cannot discover the causes of ALS? Could Hawking himself have, if not cured, perhaps contributed to his own disease’s salvation? Educated human beings place so much effort into things that will likely never save lives. And I constantly wonder if my own pursuit of mathematics will do “harm” to the world in the sense that I am not doing as much “good” as I could in chemistry.
Without a doubt, we (as a species) could have saved millions of lives from countless diseases if we had put our efforts into medical technology, instead of other pursuits. And yet we continue to do otherwise. Why? Indeed, there can only be one answer. Human lives cannot be quantified as “better” by the amount of time they exist. What I mean to say is, saving a life is not saving a life if one has instead thrown away one’s own life in the process. We are only here for a fleeting moment, and as such it is important for each of us to make the most of the fleeting moment. That may indeed consist of saving lives medically, but it may also consist of “saving lives” in other ways. Perhaps an article written by a journalist prompts a young boy to enter politics, wherein he pushes to allocate more money to NASA, who in turn create a nano-scale polymer to shed heat on rockets reentering the atmosphere, but indeed that nano-scale science is published and gives medical researchers the ability to create cancer-targeting drugs, wherein countless lives are saved. The journalist, perhaps dead for twenty years, has just saved lives, by doing what she loved best. A scenario like this, can be represented by the butterfly effect, which states that the smallest change in initial conditions can have unforeseeable consequences for the future.
In the end, then, we can at least agree that our actions, however we decide to make them, will certainly change, and possibly even save, lives. Stephen Hawking may likely still be bringing about his disease’s salvation, just in an obscure way. But at the same time, he is following his own path and immensely impacting the world for the better. It is not only our right, but our duty to pursue our own passions, even at the extent of others’ deaths.
The Singularity of Hawking’s ALS
Stephen Hawking’s life with ALS shows how much the disease varies, and how little we still know about it.
When Hawking came down with ALS in 1963, Cambridge University told him he had two years left to live. More than fifty years later, the fate of a patient is the same. We have developed only one drug for ALS, and that merely gives people three extra months.
Most people get ALS in old age and have a few years to live. However, a small percentage of people, like Hawking, get ALS when they are young, and for some unknown reason these people can live ten years or more. This makes some sense because young people are more resistant to disease in general, but Stephen Hawking has shocked the world by living to the age of 75.
The simple answer to Stephen Hawking’s survival is that he can still breathe and eat. It is possible for someone to live without use of their arms and legs, but ALS gets really difficult when other more important muscles start to atrophy. (The human heart is a special exception because it can beat without any communication from the brain.) People with ALS usually die from suffocation or dehydration due to paralysis of the diaphragm or the swallowing muscles. Stephen Hawking gets round-the-clock care, but he is known to have breathing difficulties, and he has been on a ventilator several times in recent years.
Why are the most important muscles in the body the last to break down? It really comes down to the neurons that control these muscles. For some unknown reason, the neurons that control voluntary muscles are more vulnerable to ALS than the neurons that control automatic bodily functions like digestion and bladder control. It is possible that ALS causes some neurons to become overactive and poison themselves. The only current treatment for ALS, Riluzole, is able to calm neurons down and make them live a little longer.
Other neurons are especially resistant to ALS. Research has shown that the nerves going to the eyes are resistant to hyperactivity. Stephen Hawking can still move his eyes, which is normal in the end stages of ALS. He can still smile, and he communicates via his electronic voice by twitching a muscle in his cheek. Maybe his neurons are able to stay calm.
ALS is a highly variable disease. We can describe several types of ALS, but not all cases fall into categories. With his lifespan and incredible mind both untouched by ALS, Stephen Hawking’s case is like no other.
5 Ways to Reduce Your Anxiety
Stress and anxiety are normal aspects of life. They are biological safety mechanisms that have been put in place to protect humans from dangers that threaten life and well-being. When we are in danger, our sympathetic nervous system (SNS) becomes fired up. This activates a chain reaction of neuroendocrine signaling which starts with the release of corticotropin-releasing factor in the hypothalamus of the brain and ends with secretion of stress hormones called glucocorticoids in the adrenal gland. And while we aren’t being chased by wild tigers anymore (hopefully), anxiety-related disorders are disturbingly common. According to the National Institute of Mental Health, in any given year around 18.1% of the American adult population will experience some subset of an anxiety-related disorder (1). So it is not only important to recognize when you’re anxious, but also know what to do when you have trouble calming yourself down.
Distract yourself
When anxious thoughts arise don’t dwell on them, do something else that takes away your attention from what is making you anxious. The distraction can be anything from a menial task to a hobby.
Eat healthy
Several studies have linked healthy diets that include a variety of nutrients such as foods rich in zinc, magnesium, and B vitamins with a reduction in anxiety (2). What may link anxiety and diet together is the gut-brain axis and the release of serotonin when food is injested.
Think through your anxiety
Thinking logically about what you are feeling anxious about is a tried and true method of reducing anxiety symptoms. Remember: anxiety is based on irrational thought. So it is likely what you are becoming anxious about is either not that big of deal or can be solved in some manner. In fact, the cognitive-behavioral model of psychological treatment is based on this line of reasoning (3).
Exercise
While many, including myself, find it difficult to fit in time for daily exercise, the benefits of continuous exercise on health cannot be underestimated. And while the link between exercise and anxiety isn’t clear, it has been found that symptoms of anxiety are greatly reduced when people exercise regularly. One proposed mechanism of this is through the release of ‘feel-good’ hormones during exercise like endorphins and endocannbinoids (4).
Talk to friends, family, or professionals
Strong social support networks are some of biggest indicators of good physical and mental health. Numerous studies have indicated that social support reduces the risk of developing anxiety and even modulates the symptoms of anxiety. Other studies have also shown that social isolation was linked with increased heart disease and stress levels. So when you are feeling anxious, just being able to talk to someone can help you put things into perspective and receive help.
Sources:
- https://www.nimh.nih.gov/health/statistics/prevalence/any-anxiety-disorder-among-adults.shtml
- http://www.health.harvard.edu/blog/nutritional-strategies-to-ease-anxiety-201604139441
- https://www.adaa.org/finding-help/treatment/therapy
- http://www.mayoclinic.org/diseases-conditions/depression/in-depth/depression-and-exercise/art-20046495
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2921311/
Should We Try to Prevent PTSD?
Post-traumatic stress disorder is a debilitating mental illness formed after a painful or terrifying experience. Many different situations can trigger PTSD, but there is a large concern for the prevalence within the military. Some of the situations our troops experience are unimaginable, and it shouldn’t come as any surprise that they can have lasting effects on psychological well-being. So, the big question is, how do we stop this phenomenon and protect our troops?

It is important to first understand the mechanisms underlying PTSD before answering this question. Ever noticed how the strongest memories you can recall are often from emotional experiences? That is because the brain releases specific stress hormones and neurotransmitters in response to stressful stimuli. These molecules go on to activate different regions in the brain which are important for forming memories – specifically, the hippocampus and the amygdala.
The purpose of these memories is to better prepare ourselves in case these types of situations occur again, sort of like a defense mechanism. However, extremely traumatic experiences can overactivate our stress response, or the “fight or flight” response of the sympathetic nervous system, by releasing higher levels of signaling molecules such as glucocorticoids. This results in powerful memory formation and consolidation. When triggers occur later, the brain struggles to differentiate between reality and the associated memory, setting off the sympathetic response again.
This can be especially problematic for returning soldiers as they have been conditioned to react much differently to common stimuli than the average citizen, often making it difficult for them to readjust. This brings us back to the question that arose earlier: what can we do to stop this from happening?
There are a number of treatments for PTSD, including medications (SSRIs, SNRIs, Benzodiazpines, etc.), exercise, and therapy, but the main issue with treating soldiers is the timing of when they are treated. Currently, soldiers are treated once they come back home after reporting symptoms… What if we treated them before they were deployed? Would this prevent consolidation of painful and traumatic memories? Is that a good idea?
Let’s think about this for a minute. Treating soldiers with medications before, or deploying them with medications to take while they are there, MIGHT prevent them from developing PTSD. Would this be ethical? In my opinion, no. Medications should not be prescribed before there is any need for them, putting the individual at unnecessary risk for dependency. Other side effects also need to be taken into account. Medications would decrease the stress response prior to being exposed to the stimulus. This may cause troops to react inappropriately, if at all, to high-stress situations that put their lives in danger. One wrong reaction may be fatal, and so it is important for such responses to be functioning while in combat.
I believe this issue refers less to the traumatic experience itself that results in PTSD, and more-so to the aftermath of the stimulus. The reactions troops learn while deployed are necessary for their survival. Therefore, treating them with medications before or during their deployment would be detrimental. Some possible solutions may lie in discovering a way to remove emotion and stress responses associated with specific memories, or implementing more extensive entrance testing for possible genetic precursors. However, even if an individual is not predisposed to genetic risk factors, there is still a chance that PTSD can develop. And I think it makes sense – some of the things our troops witness and experience are utterly horrific. I’m not so sure it would be a good idea to find a way to prevent people from responding to these experiences. But, I do think there needs to be a lot of improvement in the medications and other treatments we currently use. Our soldiers give so much to our country, protecting us by putting their lives on the line. It’s about time we started giving back to them.
Need Another Reason to Exercise? Stress Relief!
In some people, stressful events can be so impactful on a person’s life that their psychological, behavioral, and cognitive responses can be compromised or changed. Currently, it is understood that people who are anxious tend to form stronger memories than those who are less anxious. Because of this, mental health disorders like anxiety or PTSD can be attributed to strong memory formation from stressful events that cause long-lasting effects on behavior. A molecular mechanism that outlines the relationship between stressful events and strong memory formation is outlined in the paper we read for this week and goes as follows:
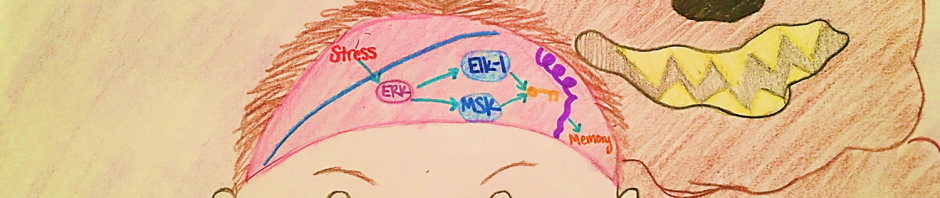
- A psychological stressor activates the ERK-MAPK pathway in a neuron.
- The activated ERK uses its kinase ability to phosphorylate two other nuclear kinases, Elk-1 and MSK, thus activating them.
- Activated Elk-1 and MSK are able to modify the chromatin through the addition of a dual histone tag, resulting in an open conformation of chromatin that allows for gene transcription.
- The new conformation allows the transcription of two immediate early genes that are known to consolidate event-associated memories.
- Thus, stressful events can induce strong memory formation through epigenetic regulation, resulting in long term behavior modification.
So how does exercise fit into stress, anxiety, and memory formation?
In an animal model, rats that participated in voluntary exercise showed increased GABA synthesis capacity, which was correlated with reduced ERK-MAPK pathway responses. This could mean that exercise increases levels of GABA synthesis capacity, which ultimately reduces the strong memory formation of stressful events, effectively regulating anxious behavior in individuals.

But exercise also releases good neurotransmitters too! Endorphins are the feel-good neurotransmitters of the brain that are in high supply during physical activity. Endorphins act as natural painkillers and are able to reduce stress by improving the ability to sleep. Those with stress, anxiety or depression are often subject to disrupted sleep due to their condition, so exercise can greatly effect emotions simply through the ability to sleep more soundly. Furthermore, anxiety or depression is 25% less likely to develop in a person who participates in regular, vigorous exercise.

Here are some tips on incorporating exercise for the purpose of stress relief:
- Pick something you enjoy doing– it seems simple, but if you pick an exercise that you enjoy you will be more likely to keep doing it as a long term commitment, rather than getting bored after a couple of weeks of an exercise you don’t like.
- Set attainable exercise goals– they can be big or small!
- Make it a time commitment– try to work exercise into your schedule by writing it in your planner, then you don’t have the excuse that you don’t have time to exercise.
- Find a friend- exercising is always more fun with a buddy, and then you have someone to keep you accountable!
- Distract yourself with your favorite music/podcast/audiobook while you exercise.
In addition to the overall health benefits, incorporating exercise into your schedule is especially beneficial for activating neurochemicals that are involved in the body’s stress response!
Anxiety and College Students: Finding a Balance
Everyone experiences stress at different times in their lives, whether it has to do with school, work, family, or just life in general. Stress isn’t always a bad thing, as it can increase our awareness and survival instincts if we are in a situation where we need to survive. Too much stress can be debilitating though, and long-term psychological stress can impact behavior and gene transcription as certain hormones, glucocorticoids, are released in higher amounts, and cause a cascade of events in the cell. These epigenetic processes may contribute to the etiology of certain stress-related mental disorders such as major depressive disorder and anxiety disorders. Anxiety and depression also have high comorbidity with each other.
Today on college campuses, anxiety is the top presenting concern among students (41.6%), followed by depression (36.4%) according to a 2013 American Psychological Association survey.

Anxiety and depression in students has started to receive more attention. Ways this has happened include events such as Mental Health Awareness days or weeks, educational days, and students are urged to open up about their experiences to others to make them feel like they are not alone and have people to talk to. Counseling Centers are now found at essentially all college campuses with services available to all students to help them with psychological issues they may be struggling with. Students are seeking to end the stigma surrounding mental disorders, and I think that this is a great thing!
I also think that that students are being “over-diagnosed” with anxiety disorder. There is a difference between having an anxiety disorder and being anxious. Students get anxious about homework, tests, relationships, etc. And yes, this can be difficult for them as they seek to balance all aspects of their lives, but it is not the same as generalized anxiety disorder, as those people are anxious all the time for no apparent reason. I think that some students think they need anti-anxiety medications to deal with the stress in their lives, when really they do not have a disorder.
I think we need to be careful trying to accommodate everything to students and trying to protect them from all things that may cause them stress and anxiety. After college when they have jobs, or are dealing with stressful situations brought about by life, they need to be able to function and deal with things without always having help from others.
If students grow up and go to college being able to avoid things that make them feel anxious, or always have accommodations for them, how will they be expected to feel like they can deal with stressful events later in their lives??
I very much understand that it is very hard for people who suffer from anxiety or feel anxious to deal with their feelings, but that is why I think that there should be more of a focus on helping students cope with their feelings when they feel anxiety coming on. Instead of just accepting that they feel anxious and trying to get anti-anxiety medications or have special academic accommodations, I think that there should be an emphasis on empowering students to help them work to become mentally stronger and learn ways to ease the effects of anxiety.

The Fallacy of Drug Scheduling
And by drug scheduling, I mean that of the United States Food and Drug Administration. And by that of the United States Food and Drug Administration, I mean listing drugs as schedule I (i.e. ‘no medical uses’).
This is not a political rant, for even prescription drugs (in the wrong hands) can be illegal, and there are good reasons for making substances illegal. But just because a substance should not be used recreationally, does not imply that it has no medical uses. We know this, of course, from the legal (yet recreationally abused) drugs such as hydrocodone, oxycontin, Adderall, etc.
Drugs, by their very nature, affect body chemistry to elicit a response. Whether this response is the elevated awareness after a cup of morning coffee, or the stark opposite of a late-night’s beer, drugs are meant to change the way we feel about the world. To label any drug as having ‘no medical uses’ is to change the definition of drugs. While I may digress into philosophy, the Hedonists of ancient Greece would support the claim that all drugs are medicines, and are we truly so knowledgeable as to say we know every possible use for a single substance?

Okay, I sound like a hippie. I apologize. This is not where I mean to lead. Instead, I am arguing for more research on drugs, even illegal drugs. While ‘no medical uses’ may be the FDA’s criterion for schedule I, I argue that the new criterion should be ‘no medical uses yet discovered’. This criterion emphasizes that many compounds, in the right context, may have the ability to change lives for the better. By scheduling some compounds as illegal, we frighten researchers into avoiding life-saving chemicals.
Perhaps the most apt example of this is the recent upsurgence of medical marijuana, and its active compounds THC and CBD, the latter of which provides no ‘high’, but can still medicate many ailments.
Even further, Anxiety and PTSD are extremely prevalent ailments to our nation, and the drugs used to treat them are not always effective. PTSD has been shown to be treated with MDMA, but its legal status renders it nearly impossible to study, let alone administer. And while no illegal drugs have been found to alleviate anxiety as a blanket disorder, there are of course subsets to anxiety disorders. One of these, most often found in advanced stage cancer patients, is the anxiety associated with a fear of death.

A recent 2011 study observed the effects of psilocybin, the active ingredient in psychedelic mushrooms, on anxiety levels of advanced cancer patients with a fear of death. The results showed a significant reduction in the patient’s anxiety over the evaluated period as shown by the STAI (an anxiety test), which was sustained over 6 months from only a single treatment.[1]

Along with that, in 2010 a population of twenty individuals suffering from medium-to-severe PTSD were half given a placebo, and half given MDMA (the pure form of ecstasy/molly), and then participated in psychotherapy sessions. The control group was later allowed to participate in the MDMA-assisted sessions two months after the set of initial trials. There was a greater than 30% decrease in CAPS scores (a PTSD test) for MDMA-assisted psychotherapy, and the few who had earlier not been able to work because of PTSD were able to work after the study had finished.[2]

Both of these drugs are serotonin agonists, which means they bind and activate receptors in the brain that serotonin would have normally bound to. As such, realizing that these are treatment options for anxiety-related disorders can tell us something about anxiety itself: that it may result from specific brain regions having low serotonin levels. It is well-known that other anti-anxiety drugs also include serotonin agonists, but regardless, we see the positive effects of schedule I drugs on patients as well as their effects on increasing our knowledge of psychological disorders. It is for just this reason that I argue to, at the very least, change the criterion for scheduling drugs, and allowing more research to be performed on them.
The fallacy by which I title this post is as follows: An illegal drug is illegal because it has no medical uses. Because the drug is illegal, it cannot be studied. Because it cannot be studied, we cannot know if it has any medical uses. Therefore, it should be illegal.
Circular reasoning. Good job FDA.
_______________________________________________________________________
[1] Grob, Danforth, Chopra, Hagerty, McKay, Halberstadt, Greer. Archives of General Psychiatric. 2011.
[2] Mithoefer, Wagner, Mithoefer, Jerome, & Doblin. Journal of Psychopharmacology. 2010.
How Stressful Memories Contribute to Anxiety
Think back to your most vivid memory. I would guess you can remember just about every detail about that situation. What time of day it was, where you were, what happened, and how you felt. Chances are, it probably is a stressful memory.

We tend to remember stressful events in great detail but it is probably to our benefit for us to remember some stressful events. Knowing what put you in danger one time will help you to avoid that stressful situation a subsequent time. In fact, when experimental rats were given a substance that decreased their anxiety, they were able to remember less about a stressful situation when put in it again.
In your brain, there is an area called the hypothalamus, which is vital to forming memories, especially contextual ones, and plays some role in responding to stress. When you’re in a stressful situation, hormones called glucocorticoids are released into particular areas of the hypothalamus. The release of these glucocorticoids is vital for the formation of memories related to stressful situations that may keep us safe. The glucocorticoid release triggers effects in the cell that lead to a change in the shape of our DNA structure that makes it easer to read genes that contribute to memory formation.

That’s all fine and good when it goes right, but what about when it doesn’t? For people with anxiety, the glucocorticoid hormones are released more often and in higher concentrations, leading to stronger memory formations, even in non-stressful situations. These anxious people that are already forming stronger memories are more likely to develop PTSD as a response to events of extreme stress.
The good news is that there are ways to prevent this stressful memory formation. Anti-anxiety drugs like Lorazepam have been shown to reduce anxiety by blocking the changes to DNA structure elicited by stressful situations. Similarly, regular exercise has also been found to inhibit the changes in DNA that lead to stressful memory formation. I’m not suggesting that exercise is the ticket to treating anxiety but it certainly can’t hurt when it is in combination with drug treatment and therapy.

Understanding these molecular markers of anxiety will hopefully help scientists in the future to develop medications that may be more effective in treating anxiety disorders and PTSD. In the meantime, knowing that there are major structural changes to DNA in people with anxiety can help us to be more understanding to those living with anxiety when we are able to realize that they cannot do anything to control this phenomenon from happening.
PTSD in the US Military
PTSD is very common among military men and women. Because they are often found in high stress, intense life-or-death situation, they experience traumatic events at a higher rate than the average person.
PTSD uses a pathway in the brain that links fear to memories. This system is evolutionarily beneficial so that when we live through a stressful or traumatic event, we can process it and handle it better the next time. However, if this circuit is imbalanced, thinking about the traumatic events or a trigger stimulus can cause the body to go into stressor mode.
In the case of the military, each applicant must go through the military entrance processing station (MEPS) to get cleared for duty. This exam includes a mental health portion. However, after service according to the US Department of Veterans Affairs, 20/100 veterans from the Operations Iraqi Freedom and Enduring freedom have PTSD. It is important to note that sometimes PTSD symptoms can appear years after the traumatic event.
In order to treat PTSD, we have combination treatments involving therapy and medications such as benzodiazepines. In 2010, the DOD Pharmacoeconomic Center reported that 20% of the 1.1 active duty US troops are on some sort of antipsychotic medication. The problem with medication is that often times, because troops have many problems including insomnia, anxiety, depression, and PTSD, a cocktail of prescribed drugs can have adverse effects including substance abuse, homicidal and suicidal thoughts.
How come everyone does not experience PTSD?
This is a tough question to answer. Each person experiences different events in combat, some more traumatic than others. Some people are also more susceptible to mental illnesses such as anxiety and PTSD. This is because of something called epigenetics, or the way DNA is read and transcribed in the body. This differs in each person and is a result of their environment and exposure to different things such as stress, or second hand smoke.
What can we do about it?
We need to monitor and modify treatments for each person so that overmedicating does not occur and each patient individually. The hard thing about mental illnesses is that it varies for each person so it is important to find the right treatment plan.
We also need to continue to de-stigmatize mental illness among military populations. While in the last few years there has been a lot of progress in this area, we need to continue to reach out and educate about these issues. I think that incidents of mental illness in the military are underreported due to the stigma. If we can educate about mental illness and stomp out the stigma we can provide care and treatment plans to those that need it.
For more information: http://www.ptsd.va.gov/public/PTSD-overview/basics/how-common-is-ptsd.asp
School Test = Bear Attack
We are living in a higher state of anxiety than we were biologically made for. Our brains were made for us to remember stressful situations that would help us to save ourselves. Like if someone died, maybe you’d remember what berry they ate right before it. Or if a bear attacked, you’d remember what area of the woods to avoid and to run away fast. But what about all of the stressful situations we subject ourselves to now? Look at American students—we’re trained to be involved in everything, get the best grades, have friends, and still exercise and sleep. That can lend to a lot of stress! But is that stress actually helping us to survive better? Is that anxiety making us better students?

I don’t think so. With all of the stress and expectations, we just get higher strung and become really good students, but not necessarily very good learners. In the spirit of learning, let’s learn how stress affects memory!
- Stress activates a signaling pathway in the brain called ERK (extracellular signal-related kinases).
- ERK activates two transcription factors (substances that can start the copying of genes) called Elk-1 and MSK.
- Elk-1 and MSK are both used to activate a dual histone tag. The dual histone tag opens up DNA so that it can be ready to copy.
- Two immediate early genes (IEGs) and copied, which help to consolidate the stressful memory.

Since these stressful memories are consolidated, they are all associated with one another. That means if something reminds you of part of the memory, they are all called up, and your body prepares to react. This can mean that you become more anxious, and you can overreact to a situation that is not life threatening. Taking a test is not the same situation as being attacked by a bear, but your brain may not know the difference if you’re stressed.
Luckily there are some things we can do to help decrease this stressful memory creation. For example, exercising can help increase the activity of GABA in the brain. GABA is an inhibitory control, so it can help to stop the signaling pathway that makes stressful memories so powerful.