 |
|
Introduction
When I think of a hereditary gene, I often think of physical appearances such as eye and hair color. If both parents of a child have brown eyes and brown hair, then there is a particularly good chance that the child will follow suit. To my surprise, this same process is shown in the psychiatric disorder, schizophrenia. Schizophrenia is a disorder that Merriam-Webster describes as, “a mental illness that is characterized by disturbances in thought (such as delusions), perception (such as hallucinations), and behavior (such as disorganized speech or catatonic behavior), by a loss of emotional responsiveness and extreme apathy, and by noticeable deterioration in the level of functioning in everyday life.” Genetics play a crucial role in the development for Schizophrenia. If an individual has a sibling or parent with the disorder, their probability of being diagnosed with the disease rise from one to ten percent. With this knowledge it is evident that there is something going on within the genetic makeup.
What Are the Contributing Genes?
Schizophrenia has been under extensive research for a long period of time. Due to the complications that are involved with this disorder, researchers have and still are having a tough time to determine the site where gene mutations are taking place. Although the disease is severely complicated, advancements in technology have allowed for bits of new information. The breach of this new information started with a study that looked at the genetic makeup of 186 Irish pedigrees. These pedigrees all had one thing in common right off the bat and that was Schizophrenia. After scans, researchers had noticed a vulnerable location in which there was activity. This activity was occurring on chromosome 6p.
The findings that the early Irish studied provided opened for a more detailed and extensive research. Scientist who were curious about this disorder were given a target to concentrate on. Studies would continue to become more and more in hopes to gain more knowledge on this complex disease. Results started to support that chromosome 6p was in fact a location with a lot of gene activity for Schizophrenia. Researchers however have not been able to target which gene or genes are accounting for this genetic vulnerability to schizophrenia.
What’s Next?
Chromosome 6p has now been a “hot-spot” for schizophrenia research. Researchers are continuing to try and pinpoint certain genes, but progress is not coming as fast as they would like. The goal would be to eventually identify these genes which would allow for future treatments and the possible deletion of the disease. Although this would be ideal, the complexity of Schizophrenia will not be allowing for that to happen anytime soon.
Conclusion
As one can tell, schizophrenia is an overly complicated disease. This complication causes many unknowns with treatments and identifications for the disease. Studies can prove that there is a hereditary gene or genes associated with the disorder but pinpointing these genes has been impossible to date. One positive note that studies did show at least gives research an area to study and that is within the 6p chromosome. Continuing with this data it is in hopes that one day we will be able to unravel this mysterious disorder.


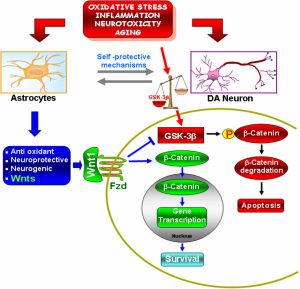
 Imagine if a skyscraper were constructed in such a way where they needed constant maintenance, and if they did not get it would be there natural state to collapse and be destroyed. It seems like a real backwards way to construct a building, or to maintain anything man-made or natural for that matter. So it is surprising to find out that a major chemical signaling pathway, the Wnt and GSK pathway, operates in manner that aligns with this metaphor. The natural state of this critical signaling pathway is that of destruction. The pathway must be activated by a Wnt ligand that triggers cellular events that stop a complex that is involved with destruction. If that seems a bit confusing, I was with you but bear with me. The pathway must be activated, to stop intracellular destruction, which maintains normal cell development.
Imagine if a skyscraper were constructed in such a way where they needed constant maintenance, and if they did not get it would be there natural state to collapse and be destroyed. It seems like a real backwards way to construct a building, or to maintain anything man-made or natural for that matter. So it is surprising to find out that a major chemical signaling pathway, the Wnt and GSK pathway, operates in manner that aligns with this metaphor. The natural state of this critical signaling pathway is that of destruction. The pathway must be activated by a Wnt ligand that triggers cellular events that stop a complex that is involved with destruction. If that seems a bit confusing, I was with you but bear with me. The pathway must be activated, to stop intracellular destruction, which maintains normal cell development.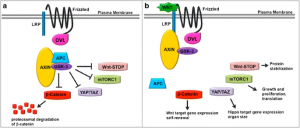




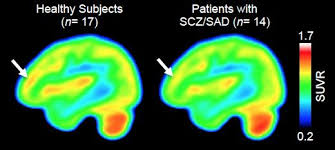



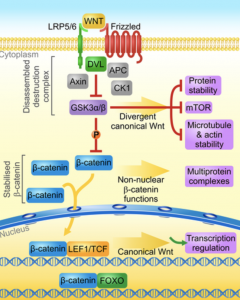 been shown to be involved with schizophrenia is the Wnt signaling pathway. When the Wnt pathway is activated it induces a cascade of events that can effect nervous system functions including neural circuit formation and synaptic
been shown to be involved with schizophrenia is the Wnt signaling pathway. When the Wnt pathway is activated it induces a cascade of events that can effect nervous system functions including neural circuit formation and synaptic 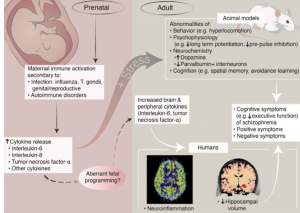 body can recruit inflammation-induced cytokines. There has been research that shows mothers who have birthed children who later are diagnosed with schizophrenia have been noted to have an elevation by nearly twofold of cytokine family molecules. Specifically, the most common cytokine family molecules that have been studied are interleukin-8 (IL8), interleukin-6 (IL6), tumor necrosis factor alpha (TNFalpha), as well as others. These molecules are soluble peptides that can cause decrease brain development and behavior abnormalities, and they have been correlated to decrease cerebral cortical neuron survival especially during brain
body can recruit inflammation-induced cytokines. There has been research that shows mothers who have birthed children who later are diagnosed with schizophrenia have been noted to have an elevation by nearly twofold of cytokine family molecules. Specifically, the most common cytokine family molecules that have been studied are interleukin-8 (IL8), interleukin-6 (IL6), tumor necrosis factor alpha (TNFalpha), as well as others. These molecules are soluble peptides that can cause decrease brain development and behavior abnormalities, and they have been correlated to decrease cerebral cortical neuron survival especially during brain 
 Lithium (yes, the element, in pill form) has been used as a treatment for schizophrenia since at least the late 19th century. It didn’t become a scientifically-based treatment until 1949, and then took another 20 years to get approval from the FDA. The fact that it wasn’t scientifically recognized didn’t stop it from being an effective treatment well before 1949 though, and amazingly, it is still used to this day as one of the most effective treatments for schizophrenia.
Lithium (yes, the element, in pill form) has been used as a treatment for schizophrenia since at least the late 19th century. It didn’t become a scientifically-based treatment until 1949, and then took another 20 years to get approval from the FDA. The fact that it wasn’t scientifically recognized didn’t stop it from being an effective treatment well before 1949 though, and amazingly, it is still used to this day as one of the most effective treatments for schizophrenia.