Feature Image Credit: Created by Jackline Peace Nanyonga using ChatGPT.
Introduction: When Energy Balance Breaks Down
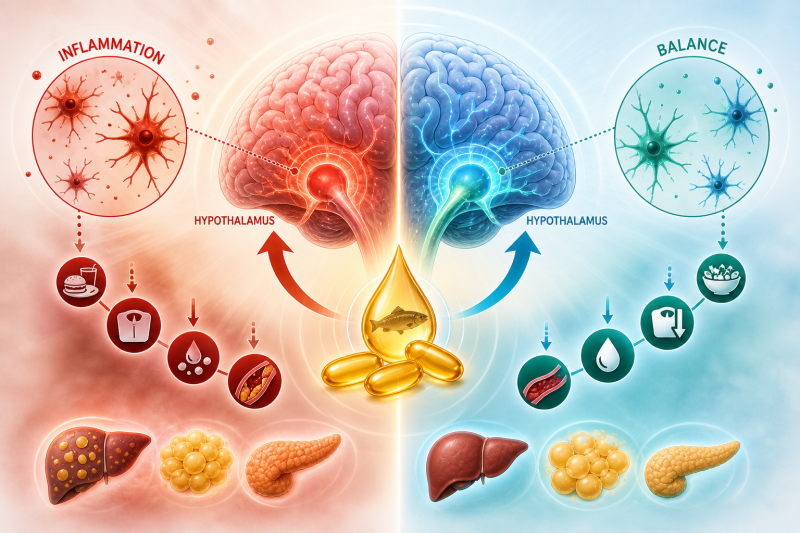
We eat to fuel our bodies and to maintain balance – between hunger and satiety, storage and use, health and disease. But in metabolic syndrome, this balance is disrupted. The body stores more, burns less, and signals get crossed. Therefore, what we eat doesn’t just add calories – it rewires the systems that control metabolism itself.
Metabolic syndrome – characterized by obesity, insulin resistance, dyslipidemia, and cardiovascular risk – is now understood as a disease of chronic, low-grade inflammation. Importantly, this inflammation isn’t just in fat tissue – it starts in the brain.
The Brain on Inflammation
At the center of metabolic regulation is the hypothalamus – a small but powerful brain region that integrates signals like insulin and leptin to regulate hunger and energy expenditure. Under normal conditions, this system maintains balance.
However, in obesity and metabolic syndrome, this system becomes inflamed.
Research shows that even a few days of a high-fat diet can trigger hypothalamic inflammation, activating pathways like JNK and NF-κB before significant weight gain even occurs.[1] This inflammation disrupts signaling:
- Insulin and leptin stop working effectively
- Hunger signals override satiety
- Energy expenditure drops
The result? A vicious cycle of overeating and metabolic dysfunction.
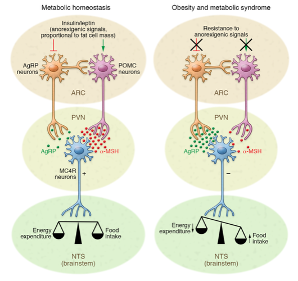 Figure 1: In metabolic syndrome, inflammation disrupts communication between hunger(AgRP) and satiety(MSH) pathways.
Figure 1: In metabolic syndrome, inflammation disrupts communication between hunger(AgRP) and satiety(MSH) pathways.
Not All Fats Are Equal
Here’s where diet becomes critical.
Saturated fatty acids (SFAs), commonly found in processed and high-fat diets, actively promote inflammation. They cross into the brain, activate immune-like pathways (like TLR4 signaling), and impair insulin and leptin signaling.[1]
In contrast, unsaturated fats – especially omega-3 fatty acids—do something different.
Instead of activating inflammation, they help reverse it.
Omega-3s as Metabolic Regulators
Omega-3 fatty acids (like EPA and DHA, found in fish, flaxseed, and walnuts) don’t just support heart health—they directly influence brain metabolism.
Studies show that omega-3s can:
- Reduce hypothalamic inflammation
- Restore insulin and leptin sensitivity
- Improve signaling in appetite-regulating neurons
In fact, experimental evidence demonstrates that unsaturated fatty acids—including omega-3s—can reverse diet-induced hypothalamic inflammation and restore metabolic signaling.[1]
Mechanistically, omega-3s:
- Inhibit pro-inflammatory pathways like NF-κB
- Reduce cytokine production
- Improve neuronal signaling related to energy balance
This essentially helps “reset” the system that metabolic syndrome disrupts.
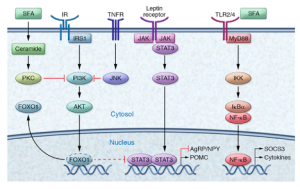 Figure 2(right): Omega-3s counteract inflammatory pathways that drive insulin resistance.
Figure 2(right): Omega-3s counteract inflammatory pathways that drive insulin resistance.
From Brain to Body—Systemic Effects
What happens in the brain doesn’t stay in the brain.
Hypothalamic inflammation affects:
- Glucose production in the liver
- Fat storage in adipose tissue
- Insulin secretion from the pancreas
This means improving brain inflammation can improve whole-body metabolism through the brain-body metabolic axis.
Omega-3s, by targeting this central control system, help:
- Lower blood glucose
- Improve lipid profiles
- Reduce overall metabolic risk
In other words, they don’t just treat symptoms—they target the control center.
Rebalancing the System
Metabolic syndrome isn’t simply a matter of eating too much – it’s a failure of regulation. And that failure is deeply rooted in inflammation, especially in the brain. But not all nutrients worsen this process. Therefore, incorporating omega-3 fatty acids offers a way to actively restore balance.
By calming inflammation, improving signaling, and reconnecting the brain to the body, omega-3s shift metabolism from dysfunction back toward regulation.
Bibliography
[1]
Jais and J. C. Brüning, “Hypothalamic inflammation in obesity and metabolic disease,” J Clin Invest, vol. 127, no. 1, pp. 24–32, Jan. 2017, doi: 10.1172/JCI88878.