Do you ever wonder why addictions seem to run in families? A parent may struggle with alcohol, a sibling with pills, and suddenly the pattern becomes hard to ignore. This is not a coincidence, it’s biology. Research shows that genetics account for 40-60% of addiction risk, shaping how our brain processes reward, forms memories, and responds to substances.[1] But genetics alone don’t tell the whole story.
How our brains reward system is already wired differently
Every brain runs on dopamine, that “that felt good, do it again” chemical. Variants in genes like DRD2 (dopamine receptor) and DAT1/SLC6A3 (dopamine transporter) influence how sensitive our reward system is and how easily impulse control breaks down.[1] Some people are simply born with a reward system tuned louder than others. That genetic difference can tilt the odds toward addiction before a person ever takes a drug, however, dopamine is only half the story.
Glutamate: The Learning and Memory Problem
Addiction isn’t just about chasing a high, it’s about learning. Glutamate, the brain’s main excitatory neurotransmitter, drives synaptic plasticity, the process by which experiences get permanently wired into memory.[2] Genes regulating glutamate receptors, including GRM5 and GRM2 (metabotropic glutamate receptors), as well as NMDA and AMPA receptors, influence how deeply drug-associated memories get carved into the brain and how hard they are to erase.
Research found. What happens to the brains Glutamate system?
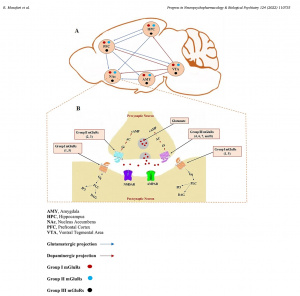 A 2023 review showed how metabotropic glutamate receptors (mGluRs) change across the brain’s reward circuit including; the nucleus accumbens, prefrontal cortex, and ventral tegmental area following cocaine, amphetamine, methamphetamine, and nicotine use. As shown in Figure 2 of the paper, mGluRs are strategically placed on both sides of the synapse: Group I receptors sit postsynaptically and drive learning-related plasticity (LTP/LTD), while Groups II and III act presynaptically as a brake on glutamate release.
A 2023 review showed how metabotropic glutamate receptors (mGluRs) change across the brain’s reward circuit including; the nucleus accumbens, prefrontal cortex, and ventral tegmental area following cocaine, amphetamine, methamphetamine, and nicotine use. As shown in Figure 2 of the paper, mGluRs are strategically placed on both sides of the synapse: Group I receptors sit postsynaptically and drive learning-related plasticity (LTP/LTD), while Groups II and III act presynaptically as a brake on glutamate release.
Repeated drug use throws this balance off. Group I receptors become overactive, fueling relapse-seeking. Group II receptors lose function, removing the brain’s natural glutamate brake. In animal studies, blocking mGluR5 significantly reduced cocaine-seeking behavior. Rats with mGluR2 deleted showed increased cocaine self-administration. Your genes controlling these receptors directly influence whether your brain pushes toward or away from relapse.
Epigenetics: When Drugs Rewrite Your Gene Expression
Through epigenetics, which is changes in gene expression without changing DNA itself, drug use can chemically silence genes involved in impulse control via DNA methylation, and alter histone modification, changing how tightly DNA is wound around proteins.[3] These changes can outlast the drug use by years, helping explain why relapse risk stays high long after someone stops using.
Why This All Matters
There are currently no FDA-approved medications for psychostimulant use disorder.[4] That’s a staggering gap. However, understanding the genetic variation in glutamate and dopamine systems is exactly the kind of knowledge that could lead to targeted treatments. mGluR-based drugs are among the most promising candidates.
Addiction isn’t a moral failure. It’s genetics, molecular neuroscience, and experience colliding in the brain. The more precisely we understand that collision, the closer we get to stopping it.
[1] “Is Addiction Genetic?,” Cleveland Clinic. Accessed: May 01, 2026. [Online]. Available: https://health.clevelandclinic.org/is-addiction-genetic
[2] P. W. Kalivas, “The glutamate homeostasis hypothesis of addiction,” Nat Rev Neurosci, vol. 10, no. 8, pp. 561–572, Aug. 2009, doi: 10.1038/nrn2515.
[3] A. S. Koijam, K. D. Singh, B. S. Nameirakpam, R. Haobam, and Y. Rajashekar, “Drug addiction and treatment: An epigenetic perspective,” Biomedicine & Pharmacotherapy, vol. 170, p. 115951, Jan. 2024, doi: 10.1016/j.biopha.2023.115951.
[4] R. Mozafari, S. Karimi-Haghighi, M. Fattahi, P. Kalivas, and A. Haghparast, “A review on the role of metabotropic glutamate receptors in neuroplasticity following psychostimulant use disorder,” Progress in Neuro-Psychopharmacology and Biological Psychiatry, vol. 124, p. 110735, Jun. 2023, doi: 10.1016/j.pnpbp.2023.110735.
