Cayley Borrud Artstract made with ChatGPT
When you think of metabolic disease and metabolism, do you think of the brain?

One of the most important regulators of metabolism is the brain. Metabolic Syndrome triggers a constant state of low-grade inflammation in the hypothalamus. The hypothalamus is the region that manages energy balance and metabolism. It’s the control center for hunger and energy balance making it vital that the hypothalamus has reduced inflammation. First, there needs to be an understanding of how diet affects this important brain area.
Image sourced from Jamestown Spine
But, how do saturated fatty acids cause inflammation in the hypothalamus?
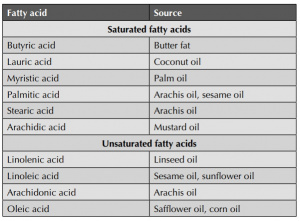
Image sourced from Pharmacy180
It starts with eating a saturated fatty acid such as pizza or ice-cream. The saturated fatty acid found in those foods, palmitic acid, is the most consumed fatty acid in the United States [2]. This activates signaling pathways and disrupts vital neuron populations [1]. Two of the most important neuronal populations involved are POMC neurons and AgRP neurons. POMC neurons help reduce appetite while AgRP neurons stimulate hunger when energy is needed. POMC and AgPR neuronal population disruptions lead to insulin and leptin resistance. This leptin and insulin resistance impairs the brains’ ability to sense nutritional cues which can then cause increased food intake and reduced energy expenditure [2]. While hypothalamic inflammation begins almost immediately, it’s very subtle. Unlike the inflammation seen in injury, this process chronic. Overtime, it disrupts the brains’ ability to interrupt hunger and fullness. Understanding these cellular interactions is vital for creating new medical strategies in combating metabolic syndrome.
Research has also shown that metabolic health may begin before birth. A maternal diet high in saturated fat may influence the developing hypothalamus of offspring. This could then increase future risk for obesity and metabolic syndrome [3]. Additionally, chronic sleep deprivation is also a major risk factor. Chronic sleep deprivation disrupts cortisol, ghrelin and leptin, therefore increasing hunger and insulin resistance [6].
What can be done to help this vital control center?
Understanding that metabolic health starts in the brain shifts the conversation from simple willpower to biological signaling. While overnutrition can cause this damage, certain factors like omega-3 fatty acids or exercise may help restore sensitivity and combat this silent inflammation [1]. Exercise can trigger anti-inflammatory signals that suppress the jammed pathways in the brain. Exercise also influences brain function by modulating the function of gut microbiota [4]. Also, Low movement decreases insulin sensitivity and reduces energy expenditure. Lower insulin sensitivity would also mean lower muscle glucose uptake [5]. Since muscle is one of the biggest regulators of blood sugar, it’s important that this system is modulated to help fight against metabolic disease.
Obesity is not simply a matter of calories. It’s deeply connected to the brains ability to regulate hunger and energy use. When the hypothalamus becomes inflamed, the body can lose its ability to accurately respond to cues of fullness therefore creating a cycle that promotes weight gain and insulin resistance. Factors such as diet, sleep deprivation and event maternal diet can influence this hidden control center. By focusing on the brain’s hypothalamic inflammation, we can work in the right direction against metabolic syndrome.
Sources:
- Jais, A., & Brüning, J. C. (2017). Hypothalamic inflammation in obesity and metabolic disease.The Journal of Clinical Investigation,127(1), 24–32. https://doi.org/10.1172/JCI88878
- skr42. (2024, August 19). Identifying ‘stealth’ sources of saturated fat, added sugar in the diet.Lombardi Comprehensive Cancer Center. https://lombardi.georgetown.edu/lombardi-stories/identifying-stealth-sources-of-saturated-fat-added-sugar-in-the-diet/
- Alum, E. U., Aloh, H. E., Obasi, D. C., Okoroh, P. N., Aniokete, U. C., & Emeruwa, A. P. (2025). Maternal nutrition, toxicants, and epigenetic programming of obesity across generations.Diabetes, Metabolic Syndrome and Obesity,18, 4873–4911. https://doi.org/10.2147/DMSO.S579409
- Sun, W., Wang, W., Zhang, Y., Liu, H., Li, L., Zhang, Y., & Liu, B. (n.d.). The brain-gut-muscle axis: A mechanism for exercise-mediated protection in brain aging.Frontiers in Aging Neuroscience,18, 1761832. https://doi.org/10.3389/fnagi.2026.1761832
- Silva, F. M., Duarte-Mendes, P., Teixeira, A. M., Soares, C. M., & Ferreira, J. P. (2024). The effects of combined exercise training on glucose metabolism and inflammatory markers in sedentary adults: A systematic review and meta-analysis.Scientific Reports,14(1), 1936. https://doi.org/10.1038/s41598-024-51832-y
- Liu, S., Wang, X., Zheng, Q., Gao, L., & Sun, Q. (2022). Sleep deprivation and central appetite regulation.Nutrients,14(24), 5196. https://doi.org/10.3390/nu14245196
